Providers should be rewarded for achieving better health outcomes.1
How we pay for coverage and care in the United States does not always provide incentives that reward value (improved quality and services at a lower cost). Instead, our system often provides incentives for higher volume, potentially leading to over-use of services and high costs. There is an need for payment reform to better align costs with health outcomes.1
Value-Based Pay for Performance (P4P) is a shared savings model that holds physician organizations accountable for the total cost, cost trend, quality of care, and resources used for all care provided to their commercial managed care members.
Indicator Highlights
A recent study indicates that as of the end of 2013, 42% of provider payments in traditional Medicare are tied to the value of care.2
The Secretary of the Department of Health and Human Services (DHHS) has set a goal of linking 85% of traditional Medicare provider payment to quality or value by the end of 2016, and 90% by the end of 2018.
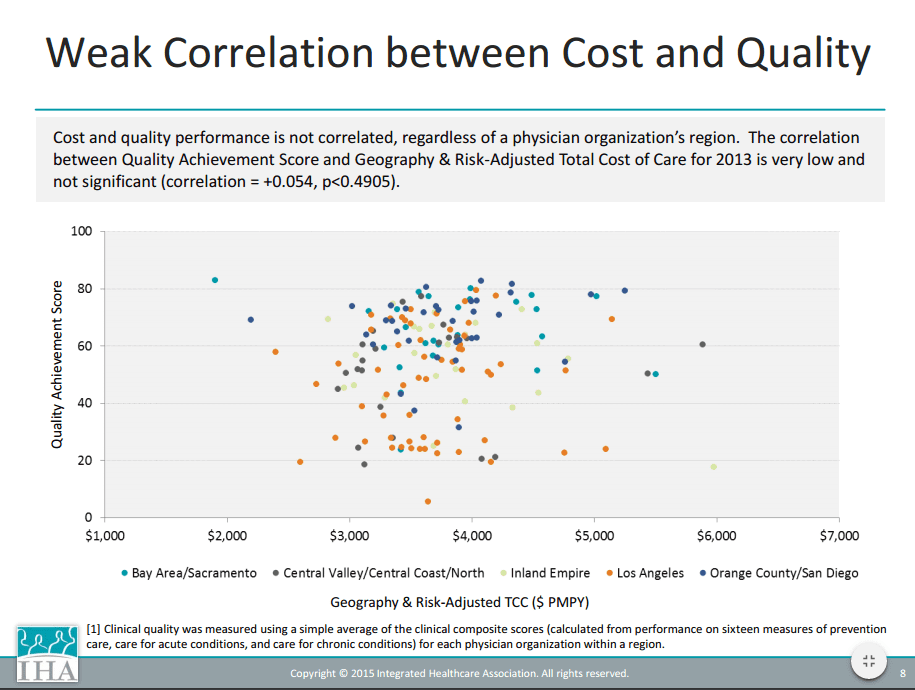
Correlation of Quality Achievement Score by Total Cost of Care by Physician Association Region
The scatter plot above shows that there is no clear correlation with Quality Composite Scores, Risk-Adjusted Total Cost of Care, and geography. Quality composite score was measured using a simple average of the clinical composite scores, calculated from performance on sixteen measures. While it may not be possible to attribute changes to the Value Based P4P program, the program may contribute to lower costs, higher quality, and less variation in both cost and quality scores as a result of systematic feedback to Physician Organizations.3
Image Source: Integrated Healthcare Association. (2015, April). Measuring Total Cost of Care. Retrieved January 7, 2016, from https://www.iha.org/pdfs_documents/p4p_california/TCC-Results-MY2013-Deck-20150427.pdf
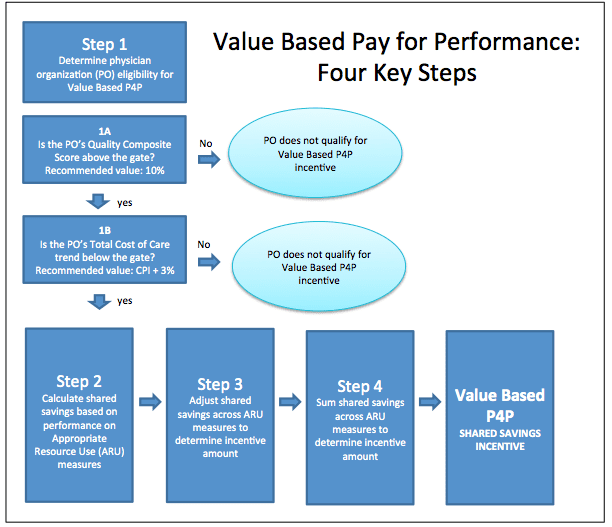
Value Based Pay for Performance in California : Four Key Steps
This flow chart illustrates the Integrated Healthcare Association’s four key steps involved in value based pay for performance.
Standardization of performance measures is a central element of pay for performance and a key advantage of the Value Based P4P design is the potential for health plans to consolidate their incentive programs into a single shared savings initiative.
|
Share Your Story
Want to engage in moving the dial on the Lowering the Cost of Care goal? Share your impact story!